Translate this page into:
Electrocardiographic abnormality in aircrew: Low atrial rhythm
Case Report
A 23 years old asymptomatic officer with an orthopedic disability reported for review to the Institute of Aerospace Medicine. The individual was asymptomatic and denied any complaints related to the cardio-vascular system. He was a keen sportsman and jogged for 7 km every day. He was normotensive, euglycemic and had no reversible cardiovascular risk factors. During the course of routine investigation an ECG was done.
Questions:
Q1. What does the ECG show?
Q2. What is your diagnosis?
Q3. How is this pathology produced?
Q4. What further investigations will you do?
Q5. What is the aeromedical concern?
Answer:
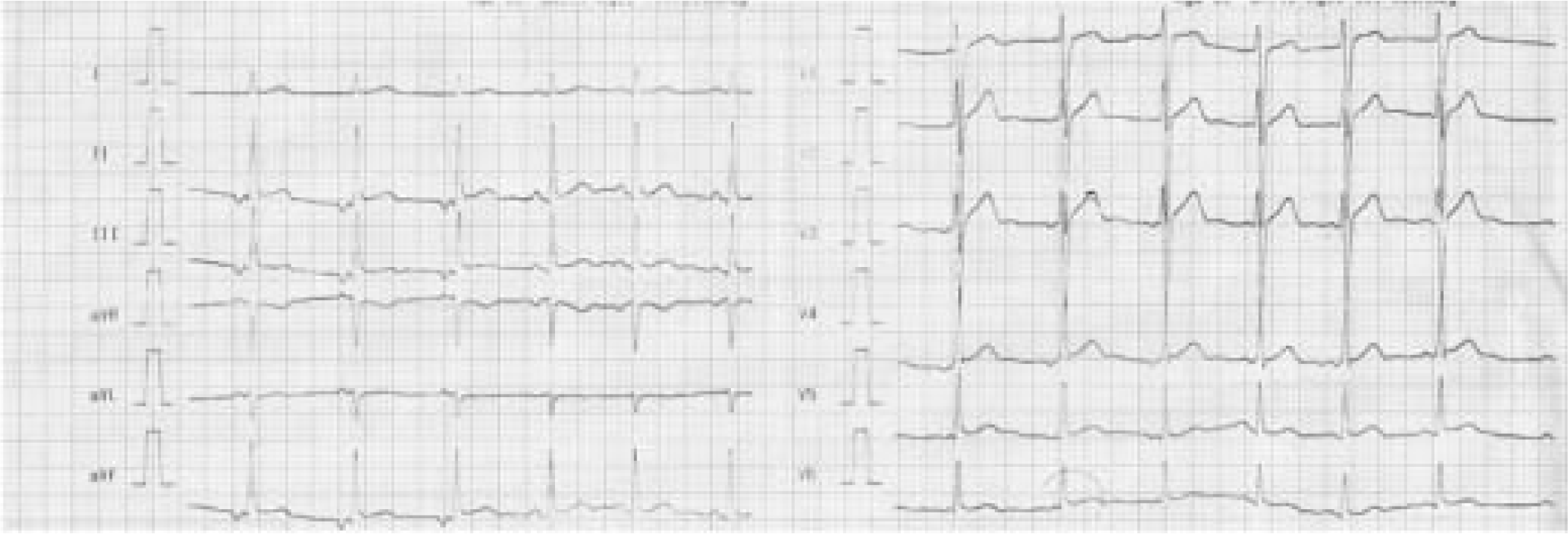
1. The conventional 12 lead ECG shows:
Pointed narrow inverted P waves in lead II, III, and aVF. A upright P wave is seen in the lead aVR.
P wave preceding a normal QRS.
Short PR interval (0.08 seconds).
A heart rate of 60 beats per minute
These changes are confined to the first two beats recorded in the ECG strip, the rest three beats shows normal sinus rhythm.
2. Low Atrial Rhythm (Retrograde Atrial activation). The activation rather than beginning at the SA node is getting initiated at an area below the SA node. This occurs when the site below the SA node usurps control from the SA node by accelerating its own automaticity, or because the SA node abdicates its role by decreasing its automaticity. The conduction to the SA node is retrograde while to the AV node it is in an antegrade fashion. The retrograde conduction to the SA node causes the inverted P waves in inferior leads while the antegrade conduction via the AV node, down is causing the normal QRS complexes. If the arrhythmia originates from within the nodal tissue, near simultaneous activation of the atrium and ventricle will occurs and the P-wave (atrial activation) may be hidden within the QRS complex and may not be noticeable on surface ECG. A low atrial rhythm refers to where the heart’s pacemaker is located. There may be several different pacemakers and when the rhythm is coming from one lower in the atrium, it is referred to as a “low atrial rhythm”.
3. The P wave, which represents atrial depolarization, is the first waveform seen in any cycle and is initiated by the sinus node in the right atrium. The atrial depolarization path therefore spreads from right to left and downward toward the atrioventricular (AV) junction. In sinus rhythm the P wave is always upright in lead I and II and always negative in AVR; in lead III, it may be upright, diphasic or negative. The AV node has intrinsic automaticity that allows it to initiate and depolarize the myocardium during periods of significant sinus bradycardia or complete heart block. This escape mechanism, with a rate of 40-60 beats per minute, produces a narrow QRS complex because the ventricle is depolarized using the normal conduction pathway. An accelerated junctional rhythm (rate >60) is a narrow complex rhythm that often supersedes a clinically bradycardic sinus node rate.
Major changes in the pattern of atrial activation, and hence the morphology of the P waves, occurs with the shift in the site of initial activation within or away from the SA node to other ectopic site. The electrocardiographic abnormalities produced includes negative P waves in the leads in which P waves are normally upright (leads I, II, aVF, & V4 through V6), with or without shortening of the PR interval. The pattern of the P waves at times can suggest the site of impulse formation; a negative P wave in lead I suggests that the origin of activation is in the left atrium, inverted P waves in the inferior leads normally correspond to a posterior atrial site. These correlations with location of origin are however highly variable. Changes in autonomic tone or the presence of sinus node disease that is causing an inappropriate slowing of the sinus node may exacerbate this rhythm.
In low atrial rhythm, depending upon the relative velocity of antegrade and retrograde conduction, the P wave may precede, follow or occur synchronously with QRS complex (hidden). Sinus P waves, at a rate equal to or slower than the junctional rhythm may also occur which may results in AV dissociation
Young healthy individuals, especially those with increased vagal tone during sleep, are often noted to have periods of junctional rhythm that is completely benign, not requiring any intervention. At times in conditions like digitalis toxicity, during acute myocardial infarction, and following cardiac surgery the AV node may develop enhanced automaticity and overtake a “normal” sinus node.
4. A 12 lead ECG forms the basis for the diagnosis. It is pertinent to note that ECG misplacement can result in similar findings and hence appropriate lead placement needs reconfirmation. All the subsequent evaluation is directed towards establishing whether the process is physiological or pathological and if pathological, the underlying etiology. The tests include –
Serum electrolyte levels: especially for individuals with comorbidities that may predispose them to accelerated junctional rhythms because of intrinsic bradycardia or AV block.
Echocardiography: for assessment of structural and functional abnormality of the heart.
Stress testing: for evaluation of chronotropic competence.
Ambulatory ECG monitoring (Holter): for assessment of arrhythmias, pauses or bradycardia.
At times when the diagnosis is still not certain, an electrophysiologic study or invasive electrophysiologic evaluation can be performed.
5. Cardio-respiratory disorders are a sinister group of disabilities and have the potential to cause sudden in-flight incapacitation. It is hence prudent to evaluate all such cases judiciously and disposed cautiously. Though no cases of low atrial rhythm in aviators has been documented the likely aeromedical concerns includes –
Low atrial rhythm may be entirely asymptomatic or may be accompanied by symptoms. The symptoms, if present include palpitation, fatigue, or poor exercise tolerance. These may occur during a period of junctional rhythm in patients who are abnormally bradycardic for their level of activity. Syncope or presyncope may also occur as a consequence of extreme bradycardia.
Low atrial rhythm by virtue of slower heart rate has the potential to lower the +Gz tolerance, in aircrew flying high performance aircraft.
Junctional escape rhythms are common in young and/or athletic individuals and occur equally in males and females. It is commonly seen during periods of increased vagal tone, for example, during sleep in younger individuals. The individual under discussion was one such case.





