Translate this page into:
Atherosclerotic Vascular Disease in Aircrew
Case Report
A 50 years old male, Navy pilot, chronic heavy smoker, reformed alcoholic, who has been physically active and claimed to be asymptomatic, reported for review medicals. He was an old case of Alcohol dependence, Diabetes Mellitus (type-2) and Dyslipidemia (on Glimepiride, Metformin and Atorvastatin), currently in non-flying category. His body weight & BP were WNL and general & systemic examinations were normal. Haemogram, urinalysis, blood sugars, lipids, serum creatinine, liver function and resting ECG were all WNL. He was due for his TMT as a routine. During TMT, he developed cramp in both legs at exercise level-3 (84% of target heart rate, 11.6 METs work load), forcing the exercise to be terminated. Symptoms subsided immediately thereafter. On questioning further, he accepted that he used to occasionally get cramps on prolonged walking (or running) which got relieved immediately on rest. ECG during stress as shown below.
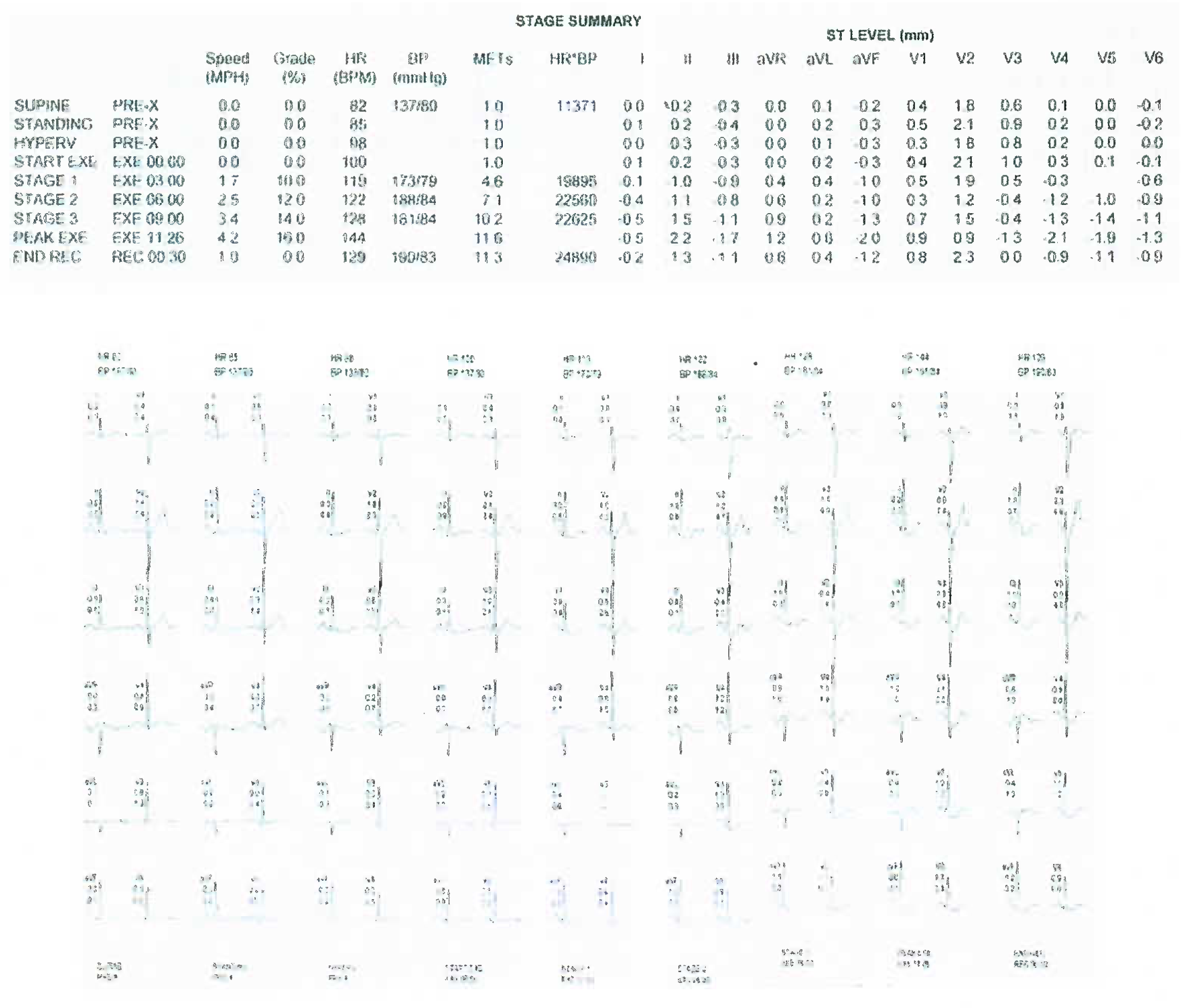
Questions:
What does the stress ECG show?
What is your diagnosis?
In view of the presented information, what other disease (not yet diagnosed) this officer is likely to have?
What further investigations will you do?
What are the major complications, this officer can develop in future?
What should be your advice to this officer?
What is the aero-medical concern?
Answers
The stress ECG shows significant ST depression (flat / down-sloping in Inferior leads (II/ III/AVF) and lateral chest leads (V5 6), maximum depression of 2.2 mm in lead-II.
In view of the ECG findings during TMT (along with leg pain/cramps induced by exertion, and relieved by rest), the TMT was considered significantly positive for ‘Reversible Myocardial Ischemia’. Along with history of risk factors, these findings led to a provisional diagnosis of ‘Coronary Artery Disease’.
The other symptom was ‘Intermittent Claudication’. If this finding is added to the history of chronic heavy smoking along with diabetes, he possibly had ‘Peripheral Arterial Disease’. The overall diagnosis becomes ‘Atherosclerotic Vascular Disease’ and it encompasses possible involvement of other important organs also e.g. CNS, retina, kidneys, mesentery etc. The major risk factors for Atherosclerotic Vascular Disease are as under:
(a) Non-Modifiable: -
(i) Male gender. Post-menopausal state in females.
(ii) Family history of premature complications of Atherosclerotic Vascular Disease.
(iii) Advancing age.
(b) Modifiable: -
(i) Hypertension
(ii) Diabetes
(iii) Dyslipidemia
(iv) Obesity
(v) Physical inactivity
(vi) Consumption of tobacco products in any form
(vii) Excessive alcohol
(viii) Stress & ‘Hot reactor’ behavior
He was subjected to following tests further:-
(a) Stress ‘Myocardial Perfusion Imaging’:- It showed a large & reversible perfusion defect in the territory of LAD artery.
(b) Coronary Angiography: - It showed 90% proximal block in LAD artery along with more sub-critical blocks in LAD, RCA and LCX. In same setting, Stenting of LAD was done.
(c) Arterial Doppler of lower limbs: - It showed severe atherosclerotic disease bilaterally, confirming our provisional diagnosis of ‘Peripheral Arterial Disease’.
(d) In addition, the officer can also be subjected to the following investigations.
(i) Fundoscopy.
(ii) Renal Doppler
(iii) Peripheral angiography, including cerebral circulation, limbs and renal circulation.
-
He is at grave risk of following complications.
(a) Chronic Angina as well as an Acute Coronary Event or even Sudden Cardiac Death.
(b) Ischemic Cerebro-Vascular Accidents (TIA or Stroke).
(c) Renal failure (acute or chronic).
(d) Arterial thrombosis of limbs (particularly lower limbs) as well as Buerger’s Disease (Thromboangiitis Obliterans). Both may lead to gangrene & loss of limb and may be life threatening..
(e) Deep vein thrombosis (DNT).
(f) Atherosclerotic disease and its complications in Retina (leading to acute or chronic visual loss which may be partial or complete).
(g) Mesenteric ischemia and its complications (gut ischemia, gut infarction etc).
Advice to this officer: -
(a) Not to consume alcohol and tobacco products (in any form).
(b) Dietary modifications in view of diabetes and dyslipidemia.
(c) Maintain regular physical activity at moderate level.
(d) Ensure timely medication and regular follow up.
(e) To be permanently placed in A4 category.
Atherosclerotic Vascular Disease can involve any or a combination of organs (mainly CNS, Heart, Retina, Limbs, Mesentery, etc). The effects may be acute, sub-acute or chronic. They have the potential to cause sudden inflight incapacitation as well as chronic disabilities. There can even be Sudden Cardiac Death. It is hence prudent to evaluate all such cases judiciously and dispose them cautiously.
| Answer Key | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| 1b | 2a | 3b | 4b | 5c | 6c | 7b | 8c | 9b | 10a |
| 11c | 12b | 13b | 14c | 15a | 16d | 17b | 18d | 19a | 20c |





