Translate this page into:
A comparative study of nasal endoscopy vis-a-vis conventional rhinoscopy in aircrew
Abstract
A comparative study of conventional rhinoscopy viz-a-viz nasal endoscopy was carried out at a boarding centre in Bangalore from June 2007 to June 2009 sampling 200 military and civil aircrew. This was done to corroborate symptoms in aircrew with findings of rhinoscopy and nasal endoscopy. Aircrew with nasal conditions like URTI, nasal allergy and past history of sinus surgery were excluded. Symptomatology was recorded and evaluation, conventional and endoscopic, performed under local surface anaesthesia. The otorhinolaryngological history taking did not reveal many symptoms initially as apparently they had no complaints. On confronting the study group with the findings after examination, nine from serving group and nineteen from civilian group accepted to have one or more symptoms of sinonasal pathology. Commonest symptom was found to be post nasal drip followed by nose block, rhinorrhoea, headache, epistaxis and anosmia. Commonest finding on conventional rhinoscopy was DNS followed by post nasal drip, nasal discharge and nasal polyps in both groups. Other nasal endoscopic findings were everted / pneumatised uncinate process, mucopurulent discharge, concha bullosa and paradoxical middle turbinates. It was observed that the presence of ethmoidal/antrchoanal polyps and post nasal drip were pathognomic of sinonasal pathology. Analysis of data revealed that a significant number of aircrew with ethmoidal polyps were missed on conventional rhinoscopy. Also mucopurulent discharge in middle meatus was significantly higher in endoscopic group.
Keywords
Nasal Endoscopy
Rhinoscopy
Introduction
The ear, nose and throat area, like many others, contains several structures that must be functioning properly for the safe performance of flying duties. It is safe to say that when these functions are impaired or exaggerated, such as eustachian tube being blocked, paranasal sinus being blocked or labyrinth sending conflicting signals to the CNS, an aircrew may become suddenly and completely incapacitated.
Some ENT conditions may be permanently disqualifying for flight, but most are either self limiting or reversible with proper treatment. Fortunately, it is uncommon for a trained aviator to be permanently grounded as a result of ENT disease or condition.
Otorhinolaryngological examination of aircrew is an integral part of aircrew selection and evaluation. It concerns organs involved in verbal communication and spatial orientation. Further, the paranasal sinuses and middle ears are semi-closed cavities sensitive to pressure variations. Verbal communication between air traffic controllers and pilots is essential for flight safety. Spatial disorientation is one of the important causes of major accidents. Barotrauma of the sinuses and middle ears can also cause considerable discomfort and distraction during aircraft descent and approach. By virtue of these unique stresses associated with aviation, otorhinolaryngological examination forms a very important component of this evaluation process.
Aim
This study was conducted with an aim to carry out a comparative study of the findings of nasal endoscopic examination and conventional anterior/ posterior rhinoscopy in aircrew and to corroborate the presence/absence of symptoms in aircrew with the findings of nasal endoscopy and conventional rhinoscopy. The objective of the study was to ascertain the contribution of nasal endoscopy in revealing the nasal pathology which are not detectable through conventional rhinoscopy and to evolve a better criteria for selection of aircrew.
Material and Methods
The present study was conducted in the Department of Otorhinolaryngology at a boarding centre for all aircrew of IAF, Navy and Army. Besides the evaluation by the department concerned with the diagnosis, all the aircrew are subjected to thorough evaluation by other departments as well. The upgradation of aircrew is considered by the medical board only after the opinion of the concerned specialist and evaluation by various other departments.
To achieve the aims and objectives a longitudinal study was designed and earned out among the aircrew reporting to the institute with problems other than those of the nasal origin.
Standard ENT evaluation equipment available were used for conventional rhinoscopy. For nasal endoscopy, Carl Storz 4mm 0 and 45 degree rigid nasal endoscopes were procured with necessary accessories.
The study was done on 200 (100 serving and 100 civilian) aircrew who had presented themselves for evaluation of various medical or surgical conditions other than nasal problems or for periodic medical examination. The aircrew subjects were in the age group of 20-54 years.
These aircrew were randomly selected as study sample from those reporting for medical evaluation at varying times. The period of study was from June 2007 to Jun 2009. All subjects had come from different geographical areas of the country, had done fair amount of flying and had reported for medical evaluation in view of their respective diagnoses. Informed consent was obtained from all subjects after counseling about the nature of study. The subjects were also given the choice to withdraw from the study at any time.
Aircrew under evaluation for any nasal condition, with recent history of URTI, postnasal drip, DNS and past sinus surgery were excluded from the study. Thus all the subjects were apparently free from any past or present rhinological disorder on the day of evaluation.
The study design was a prospective descriptive study with objective to ascertain the contribution of nasal endoscopy in revealing nasal pathology which was· not detectable through conventional rhinoscopy.
A detailed medical history was taken from each subject followed by a detailed rhinoscopic evaluation which included anterior and posterior rhinoscopy and nasal endoscopy. This was followed by ear, vestibular system, throat and neck examination in the otolaryngology department of medical evaluation centre and the findings were recorded. A comprehensive questionnaire as annexed in Appendix ‘A’ based on standard otolaryngological queries administered & feedback obtained. It had seventeen items checking on the history of present illness if any, history of past illness, family, personal and treatment history. Symptoms such as nose block, rhinorrhea, sneezing, persistent cold, post nasal drip, anosmia and ear block while flying were enquired into. History of DNS, sinus surgery, drug intake, smoking and alcohol intake was taken. History of allergies and bronchial asthma was also taken. The subjects were asked to recall impairments, if any, and respond to each item on sliding scale. It was completed at initial stage to serve as baseline and formed the basis for correlation with findings.
- Anterior Rhinoscopy

- Nasal Endoscopy
Results
The commonest symptom among the study group was post nasal drip (11%) followed by nasal blockage (9.5%), nasal discharge (8%) and headache (8%). The least common symptoms were epistaxis (1.5%) and anosmia (2%). Among the two groups, the serving personnel had post nasal drip (6%), nasal blockage (6%) and nasal discharge (5%) as the commonest symptom whereas post nasal drip (16%), nasal blockage (13%), headache (12%) and nasal discharge (11%) were commoner in the civilian group. Epistaxis and anosmia were the least common symptom in both the groups. On analyzing the symptoms among the two groups it was seen that the civilian group had significantly higher symptoms as compared to the serving group.
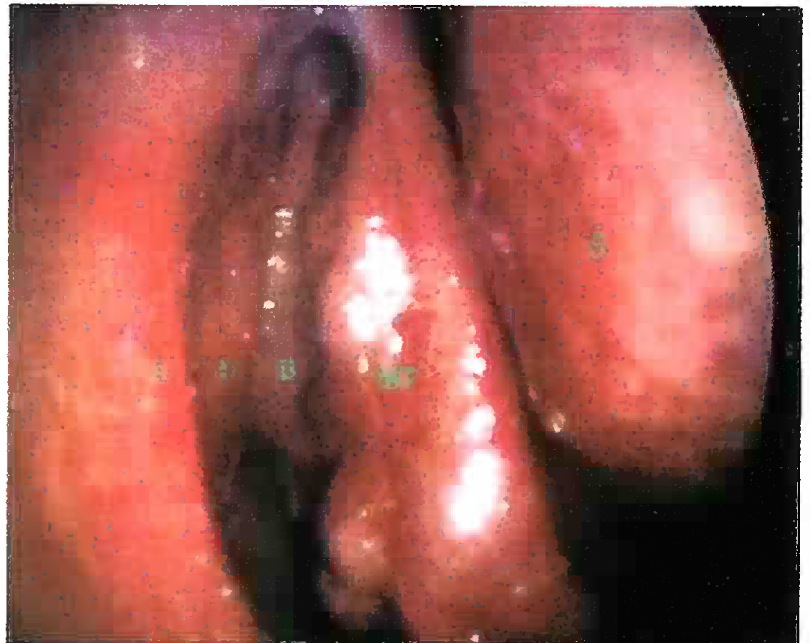
- Normal Endoscopic view of Right Nasal Cavity
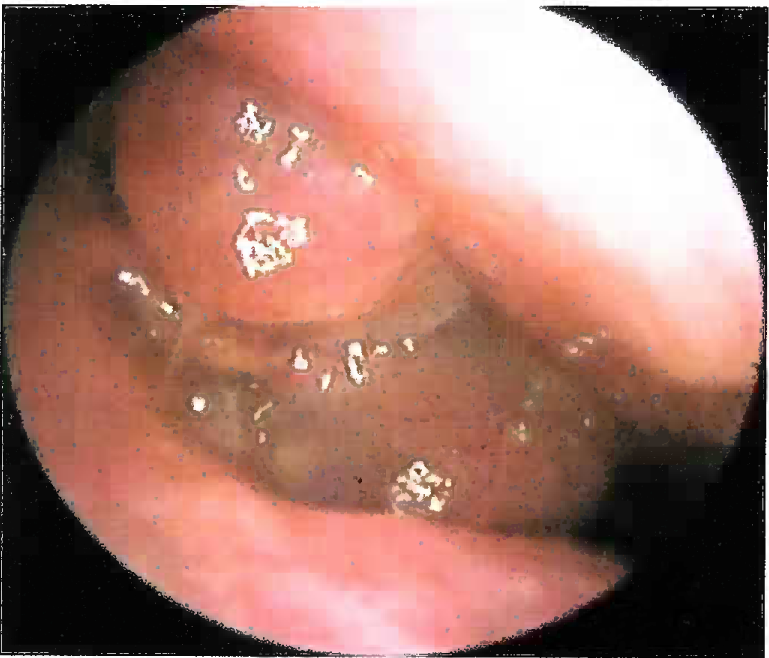
- Nasal Polyps
Conventional rhinoscopy?
Complete otorhinolaryngologic al examination was carried out in each individual and the conventional rhinological examination revealed DNS (22%) to be the commonest finding among the study group. Most of these individuals had mild DNS which was not found to have any effect on the nasal airway. On analyzing the rhinoscopic findings among the two groups it was seen that DNS and post nasal drip were significantly higher among the civilian group.
On evaluating the rhinoscopic findings among the personnel with symptoms, it was seen that DNS and post nasal drip were the commonest findings in both the groups which was followed by symptoms of nasal discharge. On analysis of the rhinoscopic findings with the individuals with symptoms, it was seen that significantly higher number of individuals who had symptoms had abnormal rhinoscopic findings.
Nasal endoscopic findings
On nasal endoscopy the serving group had concha bullosa (13%) (Fig 3) as the commonest finding followed by abnormalities of uncinate (9%) and discharge in middle meatus (6%). The civilian group had abnormalities of the uncinate process like pneumatised, everted or secondary uncinute (19%) and discharge middle meatus (19%) as the commonest finding followed by concha bullosa (11%).
On analyzing the endoscopic findings in individuals with symptoms it was seen that presence of polyps (ethymoidal and antrachoanal) (Fig 4) as well as mucopurulent discharge in middle meatus was significantly higher in individuals with symptoms. Hence these findings were found to be pathognomic findings of sinonasal pathology. On the other hand it was seen that concha bullosa, abnormalities of uncinate process and paradoxical middle turbinate did not relate to patient symptom and were found to be incidental findings on endoscopy.
On comparing the findings by conventional rhinoscopy to endoscopy on specific pathological findings that can cause sinonasal symptoms, it was seen that polyps were present in 6 individuals ( 4 ethmoidal and 2 antrochoanal polyp) as compared to 15 (12 ethmoidal and 3 antrochoanal polyp). Hence it was seen that a significant number of individuals with ethmoidal polyps are missed on conventional rhinoscopy.
Presence of nasal discharge was seen in 10 individuals on anterior rhinoscopy as compared to 25 on endoscopy. This finding of presence of mucopurulent discharge in middle meatus is pathognomic of sinusitis and was found to be significantly higher among the endoscopy group.
Discussion
In this study 200 (100 serving personnel and 100 civilians) aircrew were enrolled, at the time of their periodic medical examination or during evaluation for various other illnesses.
The study was initially started with only serving personnel. As the serving personnel are commissioned into service after a thorough medical examination, it was found that there was paucity of data both in subjective and objective parameters to reach to a conclusion. Hence 100 civilian personnel attending the same medical evaluation centre of Bangalore were included.
The otorhinolarygological history did not reveal many symptoms initially, especially in the serving personnel as they all apparently had no complaints. As most of the individuals had come for a medical examination for living, it was obvious that they would try to shield themselves and refuse to have any symptoms relating to sinonasal pathology. On confronting the study group with the findings on examination, 9 (9%) from the serving group and 19 (19%) from the civilian group accepted to have one or more symptoms of sinonasal pathology.
The commonest symptom among the study group was post nasal drip (11%), nasal blockage (9.5%J, nasal discharge (8%) and headache (8%). The least common symptom was epistaxis (1.5%) and anosmia (2%). On analyzing the symptoms among the two groups it was seen that the civilian group had significantly higher symptoms as compared to the serving group.
| Symptoms | Serving | Civilian | Total | Duration in months |
|---|---|---|---|---|
| Nasal Blockage | 6(6%) | 13(13%) | 19 (9.5%) | 03-06 |
| Nasal Discharge | 5(5%) | 11(11%:) | 16(8%) | 04-09 |
| Headache | 4(4%) | 12(12%.) | 16(8%) | 01-06 |
| Facial Pain | 3 (3%) | 7 (7%0 | 10(5%) | 03-07 |
| Ansomia / Hyposmia | 2(2%) | 2(2%,) | 4(2%) | 12-24 |
| Post Nasal Drip | 6(6%) | 16(16%) | 22(11%) | 12-18 |
| Epistaxis | 1 (1%) | 2 (2%>) | 3(1.5%)· | 01-03 |
| Conventional Rhinoscopy | Serving | Civilian | Total |
|---|---|---|---|
| Nasal Discharge | 2(2%) | 8(8%) | 10(5%) |
| Polyps on Ant Rhinoscopy | 1(1%) | 2(2%) | 3(1.5%) |
| DNS | 17 (17%) | 27(27%) | 44(22%) |
| Post Nasal Drip | 4(4%) | 11(11%) | 15(7.5%) |
| Polyp on Posterior Rhinoscopy | 1(1%) | 2(2%) | 3(1.5%) |
| Endoscopic findings | Serving | Civilian | Total |
|---|---|---|---|
| Ethmoidal Polyps | 3 (3%) | 9 (9%) | 12 (6%) |
| Antrochoanal Polyp | 1(1%) | 2(2%) | 3(1.5%) |
| Pneumatised / Everted up | 9(9%) | 19 (19%) | 28(14%) |
| Concha Bullosa | 13(13%) | 11(11%) | 24(12%) |
| Paradoxical Middle Turbinate | 4(4%) | 7(7%) | 11(5.5%) |
| Mucopurulent discharge | 6(6%) | 19(19%) | 25 (12.5%) |
After history, the study group underwent a thorough otorhinolaryngological examination including nasal endoscopy. The commonest finding on conventional filmological examination was DNS (22%). Seventeen individuals of the serving group had mild DNS which was not found to have any effect on the nasal airway. Five out of 27 civilian aircrew presented with DNS which was found to be severe enough to cause reduction in airflow. Post nasal drip was found to be the second commonest finding and was found to be higher than nasal discharge when both the groups were compared. On analyzing the rhinoscopic findings among the two groups it was seen that DNS and Post nasal drip were found to be significantly higher among the civilian group. One individual of the serving group was found to have a left sided antrochoanal polyp which was visualized both by anterior and posterior rhinoscopy. In the civilian group one individual was found to have multiple bilateral nasal polypi on anterior rhinoscopy and the other had antrochoanal polyp.
The findings on conventional rhinoscopy were compared with symptoms to correlate the subjective symptoms with objective findings. With regard to DNS, it is reported in 20-31% of the population and severe deviation has been noted as a contributing factor for sinonasal disease [1-2]. On analysis it was seen that significantly higher number of individuals who had symptoms had abnormal rhinoscopic findings. DNS (46.4%) and Post nasal drip (35.7%) were the commonest finding in individuals with symptoms.
On nasal endoscopy various anatomical abnormalities of the nasal cavities were visualized as compared to the conventional rhinoscopy. The serving group had concha bullosa (13%) as the commonest finding followed by abnormalities of uncinate (9%) and discharge in middle meatus (6%). The civilian group had abnormalities of the uncinate process like pneumatised, everted or secondary uncinate (19%) and discharge middle meatus (19%) as the commonest followed by concha bullosa (11%).
In addition to the one individual in serving group with antrochoanal polyp detected on conventional rhinoscopy, three others were found to have multiple small ethmoidal polyps in the middle meatus on nasal endoscopy. In the civilian group eight individuals with multiple ethmoidal polyps and one with antrochoanal polyp were visualized in nasal endoscopy as compared to conventional rhinoscopy. These findings present a significant increase in detection of sinonasal pathology on nasal endoscopy as compared to conventional rhinoscopy.
Discharge in middle meatus, which is pathognomic of sinusitis, was also found in a significantly higher number of aircrew by nasal endoscopy reiterating its value in diagnosing sinonasal pathology.
Some studies on the prevalence of anatomical variants have failed in identifying a significant relation with rhinosinusitis symptoms or with mucosal alterations of paranasal sinus at CT scan [3-6]. However, Bolger et al [4] have found out that the pneumatization of the bulbous portion of the middle concha presented a prevalence significantly increased in patients with sinusopathy. Likewise, larger anatomical variants present higher probability of association with tomographic alterations of paranasal sinus [7], Finally, even disregarding factors like subtype or size, Scribano et al have observed that, if the anatomical variant determines obliteration of the aerial space of the osteomeatal complex drainage paths, the sinusal disease is more frequently detected at CT than when the anatomical variant does not obstruct these pathways [8],
The prevalence of anatomical variants seems to increase with the age. Lower prevalences are found in the study including lower age ranges (1 to 7 years of age) [9]. These data suggest the hypothesis of some anatomical variants being of acquired nature. Besides the fact that in children the sinus disease is usually bilateral and symmetrical, one may infer that anatomical variants have less influence on the sinusitis etiopathogenesis in this age range than in adults [10]. Lusk et al, for example, have examined 115 children and observed that the frequency of anatomical variants was not sufficiently high to allow a statistical con-elation with sinusopathy [10].
Various studies have suggested a relationship between the presence of a concha bullosa and sinusitis [11,12], but other reports have found no direct relationship [13,14]. We in our study found no correlation between the presence of concha bullosa, abnormalities of uncinate process and paradoxical middle turbinate. The patient symptoms did not relate to these abnormal findings and were found to be incidental findings on endoscopy.
There is no consensus in literature on the role of anatomical variants in the chronic rhinosinusitis etiopathogenesis. The single detection of an anatomical variant itself does not establish the genesis of the disease. Before the suggestion of a causal relation between the anatomical variant and the sinusopathy in the tomographic analysis of a patient with sinusopathy and one anatomical variant, these conditions should be considered in conjunction with the clinical picture, its type and size, its association with obliteration of osteomeatal complex drainage paths and the presence of ipsilateral sinusal mucosa alterations.
Conclusion
This study of conventional rhinoscopy compared to nasal endoscopy in 200 aircrew revealed that very few individuals presented with symptoms; as it is a medical examination and presence of symptomatology of sinonasal disease would disqualify them.
As the serving group included personnel who were already evaluated medically before commissioning into service it was found that they had minimal symptoms and findings of sinonasal pathology as compared to civilian aircrew.
Post nasal drip and nasal blockage were the commonest symptom in both the groups with DNS and post nasal drip being the commonest findings on conventional rhinoscopy. On nasal endoscopy, significant findings were visualized in detecting sinonasal pathology especially in the civilian aircrew. Nasal polyps and mucopurulent discharge in middle meatus are pathognomic findings of sinonasal pathology and were clearly evident in nasal endoscopy.
Certain anatomical variations like concha bullosa, everted or pneumatised uncinate process and variations of middle meatus were also seen on nasal endoscopy but were not found to be significant findings of sinonasal pathology.
Conflict of Interest : None.
References
- The agger nasi cell: radiological evaluation and endoscopic management in chronic frontal sinusitis. Operative techniques. Otolaryngol Head Neck Sure. 1995;6:171-175.
- [Google Scholar]
- Role of Haller’s cell in headache and sinus disease: a case report. Otolaryngol Head Neck Surg. 1996;114:324-327.
- [Google Scholar]
- Anatomic variations of the bone in sinonasal CT. Acta Otolaryngol Suppl. 1996;525:9-13.
- [Google Scholar]
- Paranasal sinus bony anatomie variations and mucosal abnormalities: CT analysis for endoscopie sinus surgery. Laryngoscope. 1991;101:56-64.
- [Google Scholar]
- Participaçâo das variaçôes anatomicas do complexo ostiomeatal na gênese da rinossinusite crònica, analisadas por tomografia computadorizada. Rev Bras Otomnolaringol. 2001;67:489-495.
- [Google Scholar]
- Correlaçâo enologica entre variaçôes anatomicas na tomografia computadorizada e a rinossinusite crònica. Rev Bras Otorrinolaringol. 2001;67:507-510.
- [Google Scholar]
- Relationship between anatomie variations of nasal sinus and chronic sinusitis. ZhonghuaErBi YanHouKeZaZhi. 1998;33:149-152.
- [Google Scholar]
- Computerized tomography in the evaluation of anatomic variations of the ostiomeatal complex. Radiol Med (Torino). 1993;86:195-199.
- [Google Scholar]
- Tomografia computadorizada hélicoïdal dos seios paranasais na criança: avaliaçâo das sinusopatias inflamatórias. Radiol Bras. 2002;35:161-169.
- [Google Scholar]
- Anatomic variation in pediatric chronic sinusitis: a CT study. Otolaryngol Clin North Am. 1996;29:75-91.
- [Google Scholar]
- CT evaluation of the paranasal sinuses in symptomatic and asymptomatic populations. Otolaryngol Head Neck Surg. 1991;104:480-483.
- [Google Scholar]
- Influence of naso-sinusal anatomic variants on recurrent, persistent or chronic sinusitis. X-ray computed tomographic evaluation in 112 patients. J Radiol. 1997;78:651-657.
- [Google Scholar]
- The etiological role of concha bullosa in chronic sinusitis. Eur Radiol. 1996;6:550-552.
- [Google Scholar]






